
Let’s Talk!
We’re here to help you with any questions you may have. Please don’t hesitate to reach out to us.
For mild cases of plantar fasciitis, conservative management is usually effective in controlling the inflammatory process and reversing the damage (without needing any further treatments). In fact, conservative management is often effective in more than 80% of cases of plantar fasciitis, often resolving the pain within a few months.
Early initiation of conservative remedies is the key to managing your pain and inflammation while minimizing the risk of disability and chronic inflammation. The longer you experience plantar fasciitis pain or delay seeking treatment, the less likely you will improve from conservative treatment. The initial treatments for plantar fasciitis involve a combination of specific treatments with the goals being to: control the inflammatory response; limit further injury; and, promote healing.

Ice or cold compresses alleviate the symptoms of pain and discomfort. You can massage the bottom of your foot with an ice pack wrapped in a towel. Rub an ice-pack gently over the tender area on your heel for 15 to 20 minutes, 3-4 times a day.
Additionally, rolling your foot on a bottle of frozen water can also give quick relief from pain and discomfort. Ice massage can also be used as a preventative measure to minimize the attacks of pain after long periods of rest or inactivity.

Therapeutic deep tissue massage to the heel pad and back of the calf muscles is known to help the pain, swelling and discomfort associated with plantar fasciitis. When performed in expert hands, deep tissue massage helps release tension and break scar tissue. If the massage is aggressive, you may experience some pain or soreness after the massage, which resolves in a few hours or occasionally, a few days.

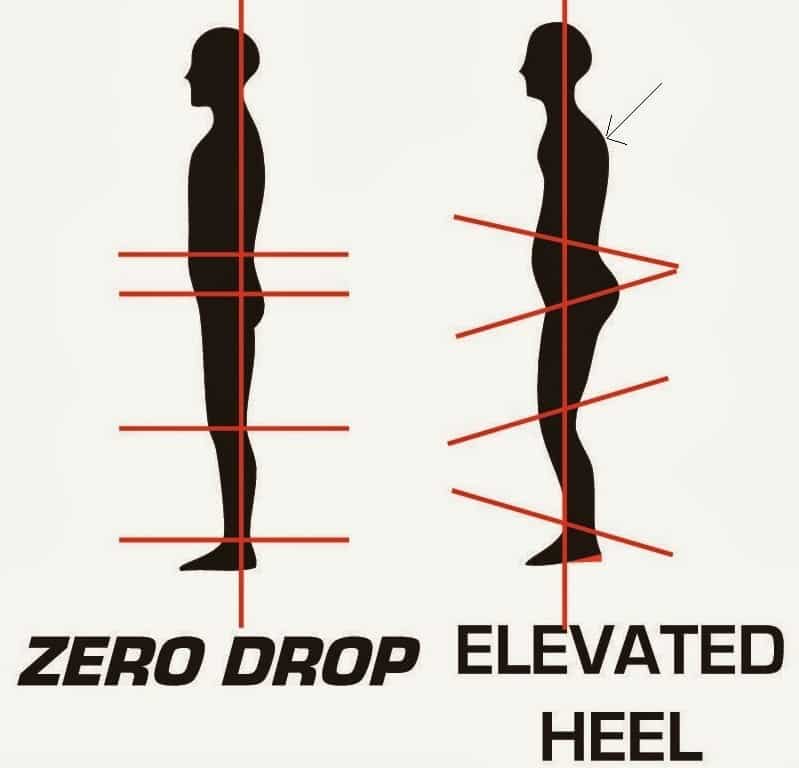
Improper footwear is a leading cause of plantar fasciitis and other foot disorders (such as Morton’s neuroma). Some footwear recommendations for patients with plantar fasciitis include:
Custom made shoes are another suitable option in special cases (such as congenital or acquired foot deformities and postural disorders of foot/ leg). Remember: wear shoes that work with your feet not against them!

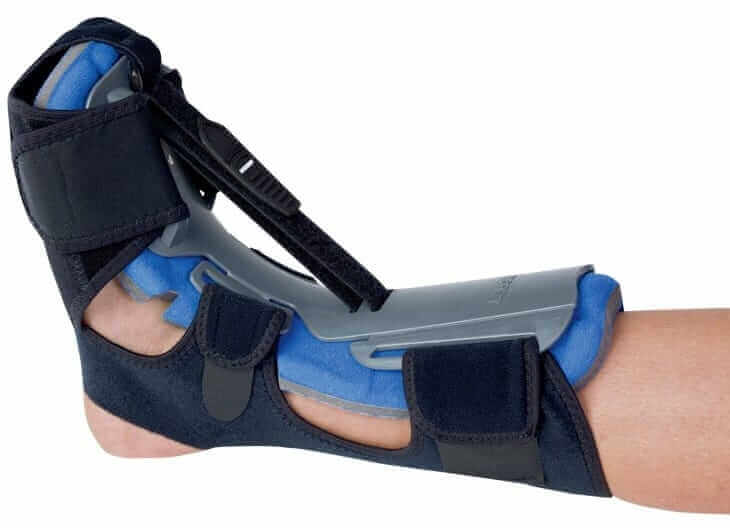
Night splints help in stretching your calf muscle and supporting the arch of your foot. The night splint assists in holding the plantar fascia and the Achilles tendon in an elongated position during sleeping to expand the fascial sheath. Night splints need to be used each night regularly and failure to wear these nightly limit their effectiveness. Poor sleepers have particular difficulty with this treatment as the splints disrupt their sleep. Various studies suggested that regular use of tension night splints with stretching, heel cups, NSAIDs and shoe modification can resolve Plantar Fasciitis symptoms completely (without needing any other therapy).
A simple way to treat the pain of plantar fasciitis is through the use of medications which are used in conjunction with other interventions such as stretching. They can help to reduce pain enough to facilitate stretching, physical therapy and exercise. However medications have a minimal role in treatment or prevention of plantar fasciitis and should be reserved for temporary use only.
They can help to reduce pain enough to facilitate stretching, physical therapy and exercise. However medications have a minimal role in treatment or prevention of plantar fasciitis and should be reserved for temporary use only.
NSAIDs have minimal role in treatment or prevention of plantar fasciitis and should be reserved for temporary use only.
We use a type of ESWT called Extracorporeal Pulse Activation Technology or EPAT® which has been shown to be very effective when used in  early plantar fasciitis. Extracorporeal Pulse Activation Technology uses high frequency sound waves that are directed at the most tender part of the heel to promote healing.
early plantar fasciitis. Extracorporeal Pulse Activation Technology uses high frequency sound waves that are directed at the most tender part of the heel to promote healing.
EPAT offers fast recovery allowing you to resume your daily living activities quickly. It is estimated that extracorporeal shock wave therapy is effective in resolving greater than 70% of cases of persistent plantar fasciitis pain. Recent studies have shown that patients with heel spurs, edema or high pain scores respond better to EPAT. The exact therapeutic mechanism of shock wave therapy still remains a topic of speculation despite extensive research. It is thought that sound waves damage tissues to induce microtrauma, which stimulates the healing process by attracting blood vessels and nutrients to the plantar fascia. The sound waves also inhibit pain receptors.
The Procedure. Our protocol for EPAT is a course of 3 treatments, each 2 weeks apart. The procedure is generally well tolerated with minimal discomfort.
Side effects are rare especially when procedure is performed in expert hands. Side effects may include: bruising, post-procedure inflammation, discomfort, pain, swelling and tenderness (all of which usually resolve spontaneously.) Contraindications to EPAT include: a history of hemophilia or other coagulopathies; malignancy; and open bone growth plates (physes.)
Relief: Many patients have pain relief immediately after EPAT. EPAT has a cumulative effect so repeating the procedure can be beneficial. The full effect each course of treatment may take up to 6 weeks.
 If conservative measures do not result in adequate pain relief then an ultrasound guided corticosteroid injection is a possible alternative.
If conservative measures do not result in adequate pain relief then an ultrasound guided corticosteroid injection is a possible alternative.
Ultrasound guided steroid injections are widely used in the management of plantar fasciitis however their use has recently declined due to the risk of fat pad atrophy. Use of ultrasound guidance helps in increasing the accuracy while reducing the risk of side effects including fat pad atrophy. One well placed steroid injection can resolve pain for a period of up to 4 weeks and minimize the risk of inflammatory swelling for up to 3 months. Studies have shown that a corticosteroid injection is more likely to be successful if the ultrasound shows peri-fascial edema.
Side effects of this procedure are; transient numbness, pin and needle sensations and localized discomfort. Repeat corticosteriod injections should be done with extreme caution since long-term steroid therapy may aggravate the risk of damage such as tearing of the plantar fascia, atrophy of the skin, heel muscles and fat pad, degeneration of tendons etc. and is therefore not recommended.
Other conservative remedies should be used in conjunction with ultrasound guided corticosteroid injections such as orthotics and stretching exercises. However, if your symptoms are not resolving or getting worse over time, you should consider other nonsurgical procedures for the treatment of persistent plantar fasciitis.
Physical therapy exercises performed under the supervision of a physical therapist help in strengthening and stabilizing the plantar fascia, Achilles tendon and Gastrocnemius muscles, which in turn, improves the integrity of the plantar fascia and other connective tissue components of lower leg and minimize the risk of injuries.
Orthotics are specialized devices that are designed to keep the curvature of the arch intact and stable and minimize existing stresses to the foot. They should recreate the shape of the heel pad and decrease excessive pronation. There are several varieties of orthotics depending upon individual needs and preferences such as cups, cushions and various insoles. They vary in level of support, correction and control. Over-the-counter orthotics are considerably cheaper than custom orthotics and great care must be taken when choosing these. Custom orthotics are considerably better especially when created by a orthotist experienced in plantar fasciitis.
Some studies show the efficacy of full length arch pads as high as 81%, silicone heel inserts 95%, and rubber heel cups is 88% while other studies show only moderate improvement. Orthotics are generally more likely to be successful in patients with flat feet who over pronate.
Low-impact activities like swimming or bicycling should be preferred over walking or jogging for those concerned about life-long recovery from Plantar Fasciitis. Low force activities decrease the impact on the arches and plantar fascia. Stretching alone or in combination with other conservative remedies is considered a cornerstone of Plantar Fasciitis management (See above). Easy home based exercises can help in stretching the plantar fascia, Achilles tendon and muscles of the lower leg. Simple stretching exercises of the lower limb help in stabilizing the ankle joint and maintain the integrity of the foot arches.
Maintaining a healthy weight and keeping a strict check on body mass index can help reduce the stress on plantar fascia. Healthy eating and daily exercise are required to maintain an optimal body mass index. Cross training with exercises involving swimming and cycling can help those with Plantar Fasciitis achieve the level of aerobic exercise to help maintain a healthy weight.
The effectiveness of taping is unclear at best. Low-Dye taping may provide temporary relief of mild to moderate heel pain by supporting the foot arches and reducing excessive pronation but is now generally considered ineffective for chronic plantar fasciitis. Furthermore, taping can be quite complex and time consuming. Do not use low-dye taping if you have a circulatory or sensory condition or an unhealed fracture of the foot. See here or here.

We’re here to help you with any questions you may have. Please don’t hesitate to reach out to us.
The Center for Morton's Neuroma
